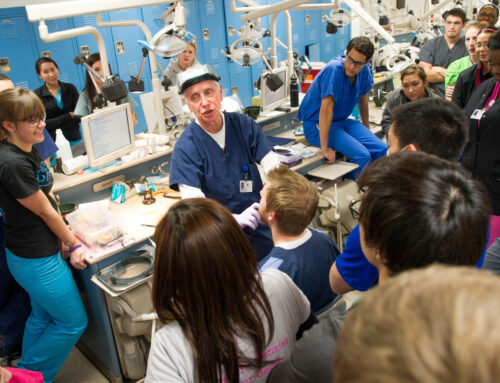
Photography by Kathy Tran.
BECKY HINES’ CLIENT never intended to give birth at home. But her husband, who was serving overseas, was barred from traveling because of the pandemic, and she was terrified of giving birth at a hospital alone.
She called Hines, a midwife, and decided to give birth at home. During labor, the woman’s husband offered support and watched the delivery via Skype.
“She had a great, happy, healthy birth,” Hines says. “We are always so thankful for the hospital, but for women who desire a different option, we’re glad midwifery is there.”
The pandemic prompted many pregnant women to reassess their birth plans. As virus cases rose in hospitals, forcing them to enact strict visitation policies, Hines and her collective of licensed professional midwives experienced a surge of interest in home births.
Hines and partners Kiesha Baker and Nikki Knowles earned their midwifery licenses early last year and founded the Dallas Birth collective, offering midwifery care, doula services, childbirth classes, lactation counseling and placenta encapsulation. They are equipped to help women give birth at home and have privileges at East Dallas Birth & Wellness center.
Additional family members, doulas and photographers are allowed at all births as long as they do not exhibit COVID-19 symptoms.
“Midwifery is becoming more mainstream,” Hines says. “It’s not just hippie crunchy granola moms who are doing it. We have new moms and women who have had babies in hospitals before but are looking for a different model of care.”
Midwives follow the same visitation schedule and offer the same routine tests as obstetricians. In Texas, they can carry medications but cannot give epidurals for pain management. They are certified to perform neonatal resuscitation and trained for emergencies. Dallas Birth partners with Baylor Hospital if a patient needs doctoral care.
“Women are looking to feel known and heard,” Baker says. “Our appointment times are one hour. When you go to an OB, it’s like 15 minutes. We’re weighing in emotionally and preparing them for all aspects of the birth — health, diet, etc. The better we know our clients, the safer we can keep them.”
Home births account for just 1 percent of the U.S. total, according to the National Center of Biotechnology Information, but the practice was common until the expansion of the public hospital system in the early 20th century.
Yet the U.S. has the worst maternal mortality rate among similarly wealthy countries, according to the Centers for Disease Control and Prevention. The latest findings from 2018 estimate a maternal death rate of 17.4 deaths per 100,000 live births. That means 658 women died.
It’s a particular concern for Black women, who are two to three times more likely to die from pregnancy-related causes than their white counterparts, according to the CDC.
“I never thought I would be a midwife,” says Knowles, who is Black. “When I was a doula, the idea of home birth was like, ‘Who does that?’ But it’s hard when you know so much about birth, you know when a person is being taken advantage of and then seeing the statistics of Black women and families. I felt like I wanted to do more. I wanted to be more involved in the care. When clients come that look like me, their shoulders drop. It’s a sigh of relief. They can be authentic and vulnerable.”
The midwives agreed that racism and biases embedded in the medical system contribute to the problem.
“I was a doula at a local hospital for a Black woman who was having her third baby,” Baker says. “She was at a place in labor where the hospital would keep her, but they were downplaying her pain and were going to send her home. I had to step in. ‘Do you want me to catch this baby?’ Sure enough, she had a baby two hours later. I’ve seen [discrimination] several times over the years. It should not be surprising, but in my white privilege, it is.”
The Midwives Model of Care takes a different approach to traditional obstetrics, providing extended, individualized care to a low number of patients. The midwives say it can work in any setting, and so far, it has. When the pipes froze at the birth center during February’s winter storm, the midwives delivered babies without running water. Another time, the electricity went out at the facility, and a mom gave birth in the dark on the bathroom floor.
“It’s been good, but also overwhelming,” Knowles says. “There’s a lot of logistics to figure out. There’s a misconception that midwives have a robe and go under a tree to deliver your baby. But, hey, if that’s what the mom wants, then that’s fine.”